Types of Alopecia Explained: From Androgenetic to Alopecia Areata
A comprehensive breakdown of alopecia types, how each progresses, and which conditions respond best to surgical vs. medical treatment.
The word "alopecia" simply means hair loss, but it encompasses a wide spectrum of conditions with very different causes, progression patterns, and treatment responses. Understanding which type of alopecia you are dealing with is not just an academic exercise; it is the essential first step toward choosing a treatment that will actually work. A therapy that produces excellent results for androgenetic alopecia may be completely ineffective for alopecia areata, and a hair transplant that delivers transformative results for one condition may be contraindicated for another.
This guide walks through the major types of alopecia, explaining the biology behind each, who it affects, how it progresses, and which treatment options offer the most promise.
Androgenetic Alopecia
Androgenetic alopecia is by far the most common form of hair loss, affecting an estimated 50 percent of men and 25 to 30 percent of women over their lifetimes. It is the condition most people mean when they say "pattern baldness" or simply "going bald."
In Men
Male androgenetic alopecia follows the well-known pattern of temporal recession and crown thinning, classified by the Norwood-Hamilton scale from Stage I (no significant loss) to Stage VII (extensive baldness with only a horseshoe ring remaining). The driving mechanism is the conversion of testosterone to dihydrotestosterone (DHT) by the enzyme 5-alpha reductase. DHT binds to androgen receptors on genetically susceptible follicles, triggering progressive miniaturization over successive hair growth cycles.
Treatment options include finasteride (which blocks DHT production), minoxidil (which stimulates follicular activity), PRP therapy (which delivers concentrated growth factors to the scalp), and surgical restoration through FUE or FUT hair transplantation. The condition is progressive and lifelong, meaning that treatment must be ongoing or the loss will resume.
In Women
Female androgenetic alopecia presents quite differently, typically as diffuse thinning across the top of the scalp without frontal hairline recession. Classified by the Ludwig scale into three grades of severity, it is influenced by the same androgens but modulated by estrogen and other hormonal factors. Treatment for women often combines minoxidil with anti-androgen medications like spironolactone, along with PRP therapy and, in appropriate candidates, surgical restoration.
Transplant candidacy: Androgenetic alopecia is the condition for which hair transplant surgery was designed, and it remains the primary indication. Both men and women with stable androgenetic alopecia and adequate donor density are typically excellent candidates.
Alopecia Areata
Alopecia areata is an autoimmune condition in which the body's immune system mistakenly attacks hair follicles, causing them to enter a premature resting phase and shed their hairs. The result is one or more smooth, round patches of complete hair loss, most commonly on the scalp but potentially affecting any hair-bearing area of the body.
Who It Affects
Alopecia areata can strike anyone at any age, though it most commonly appears before the age of 30. It affects men and women equally and occurs across all ethnic backgrounds. There is a genetic component: people with a first-degree relative who has alopecia areata are at higher risk, and the condition is associated with other autoimmune disorders including thyroid disease, vitiligo, and type 1 diabetes.
How It Progresses
The course of alopecia areata is notoriously unpredictable. Some patients experience a single patch that regrows spontaneously within months. Others develop multiple patches that coalesce, or experience repeated episodes over years. The presence of certain factors, including onset before puberty, extensive involvement, loss of eyebrows or eyelashes, and a family history of autoimmune disease, suggests a more persistent course.
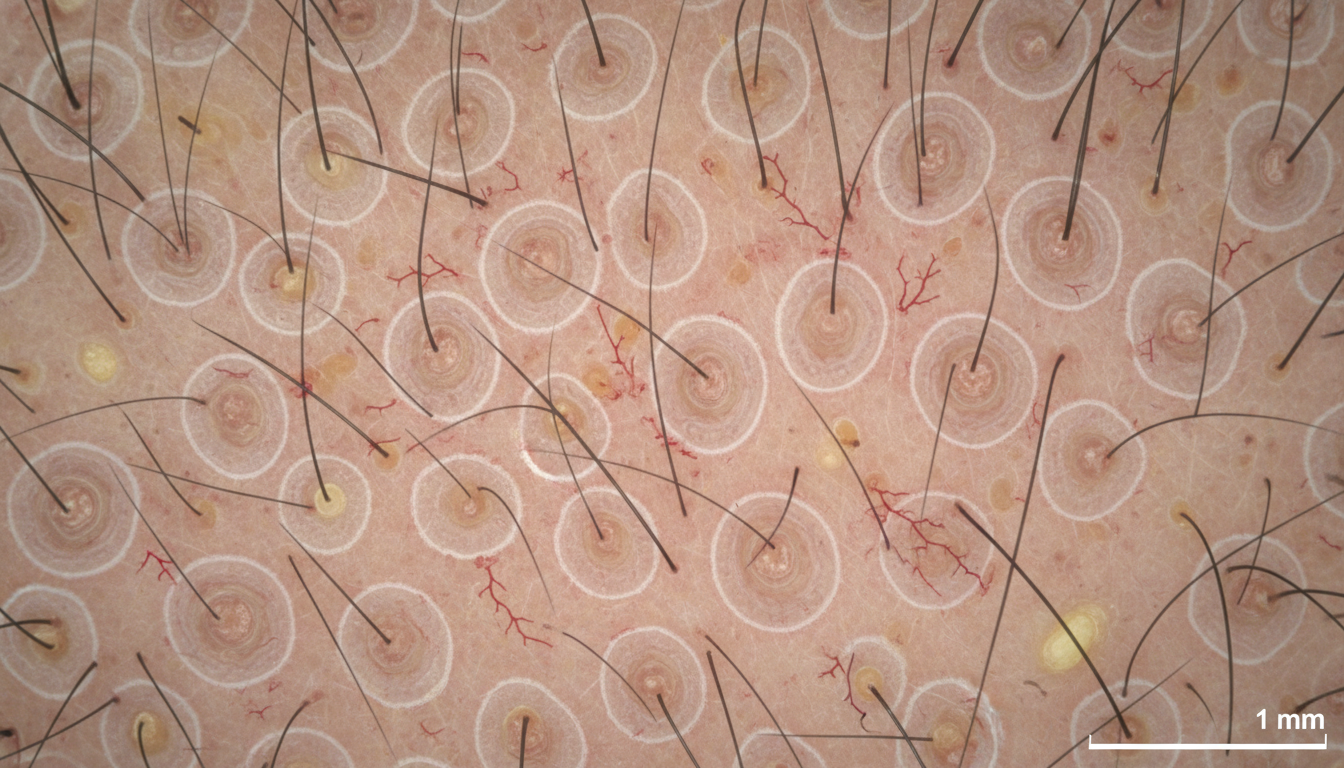
Treatment
Treatment for alopecia areata focuses on modulating the immune response. Topical and intralesional corticosteroids are first-line treatments for limited disease. For more extensive cases, immunotherapy with agents like diphenylcyclopropenone (DPCP) may be used to redirect the immune response. Newer JAK inhibitor medications have shown remarkable efficacy in clinical trials and are changing the treatment landscape for moderate to severe alopecia areata.
Transplant candidacy: Hair transplant surgery is generally not recommended for active alopecia areata. Because the condition is autoimmune and unpredictable, transplanted follicles may be attacked by the immune system just as native follicles were. However, patients with very stable, long-standing alopecia areata who have not had active disease for several years may be considered on a case-by-case basis.
Alopecia Totalis and Alopecia Universalis
These are severe variants of alopecia areata. Alopecia totalis involves complete loss of all scalp hair, while alopecia universalis results in the loss of all body hair, including eyebrows, eyelashes, nasal hair, and body hair. These conditions represent the most advanced forms of the autoimmune attack on hair follicles.
Treatment follows the same immunomodulatory approach as for alopecia areata, though the severity of these conditions often necessitates more aggressive systemic therapy. JAK inhibitors have offered the most significant therapeutic breakthrough for these patients in recent years. Hair transplant surgery is not typically recommended for these conditions due to the high risk of graft loss from ongoing immune-mediated destruction.
Traction Alopecia
Traction alopecia is caused by sustained, repetitive pulling on hair follicles from tight hairstyles. It is not an autoimmune or hormonal condition; it is purely mechanical. The constant tension damages the follicular attachment, eventually leading to inflammation, scarring, and permanent follicle loss if the traction continues long enough.
Who It Affects
Traction alopecia is most commonly seen in women who wear their hair in tight braids, cornrows, extensions, weaves, or very tight ponytails over extended periods. It is particularly prevalent in African American women due to cultural hairstyling practices, but it can affect anyone who subjects their hair to chronic mechanical stress. Ballerinas, swimmers who wear tight swim caps, and individuals who habitually pull their hair into tight buns are also at risk.
Progression and Treatment
In its early stages, traction alopecia is reversible. The hair loss appears as thinning or small bare patches along the hairline, temples, or wherever tension is greatest. If the patient changes their hairstyling practices, the follicles can recover and regrow hair. However, if the traction continues for years, the chronic inflammation leads to follicular scarring and permanent loss.
Transplant candidacy: Traction alopecia is actually one of the conditions that responds very well to hair transplant surgery, provided the patient has stopped the causative styling practice. Because the underlying follicular biology is healthy and there is no ongoing autoimmune or hormonal process attacking the follicles, transplanted hairs typically survive and grow normally in the recipient area.
Cicatricial (Scarring) Alopecia
Cicatricial alopecia is a group of rare disorders that destroy hair follicles and replace them with scar tissue, resulting in permanent hair loss. Unlike other forms of alopecia where the follicle shrinks but is potentially recoverable, scarring alopecia involves actual destruction of the follicular stem cells.
Types
The scarring alopecias include several distinct conditions:
- Lichen planopilaris (LPP): An inflammatory condition that causes redness, scaling, and progressive destruction of follicles, typically at the hairline or scattered across the scalp.
- Frontal fibrosing alopecia (FFA): A variant of LPP that causes a slowly progressive, band-like recession of the frontal hairline and often affects the eyebrows as well. It is most common in postmenopausal women.
- Central centrifugal cicatricial alopecia (CCCA): A condition that begins at the crown and spreads outward in a centrifugal pattern. It predominantly affects women of African descent and is the most common cause of scarring alopecia in this population.
- Discoid lupus erythematosus: An autoimmune condition that creates well-defined, disc-shaped patches of inflammation and scarring on the scalp.
Treatment
The primary goal in treating scarring alopecia is to stop the inflammation before more follicles are destroyed. Anti-inflammatory medications, including topical and oral corticosteroids, hydroxychloroquine, and immunosuppressants, are the mainstay of treatment. Early and aggressive treatment is critical because once a follicle is replaced by scar tissue, it cannot be recovered.
Transplant candidacy: Hair transplantation in scarring alopecia is possible but carries additional risk. Surgery should only be considered after the disease has been quiescent for at least one to two years, as transplanting into an area of active inflammation will likely result in graft failure. Even in quiescent disease, there is a risk that the inflammatory process may reactivate and destroy transplanted follicles.
Telogen Effluvium
Telogen effluvium is a reactive form of hair shedding triggered by a physiological or emotional stressor. It occurs when a large number of hair follicles simultaneously shift from the active growth phase (anagen) to the resting phase (telogen), resulting in diffuse shedding two to four months after the triggering event.
Common Triggers
- Major surgery or hospitalization
- High fever or severe illness
- Significant weight loss or crash dieting
- Childbirth (postpartum hair loss)
- Emotional trauma or chronic stress
- Starting or stopping medications (including oral contraceptives)
- Nutritional deficiencies (iron, zinc, vitamin D)
The hallmark of telogen effluvium is that it is diffuse, affecting the entire scalp rather than creating patches, and it is self-limiting once the trigger resolves. Most cases recover fully within six to twelve months. Chronic telogen effluvium, in which the shedding persists beyond six months, may indicate an unresolved underlying cause that requires investigation.
Transplant candidacy: Hair transplant surgery is not appropriate for telogen effluvium because the condition is temporary and the follicles are not permanently damaged. Treatment focuses on identifying and resolving the triggering factor, nutritional optimization, and patience.
Anagen Effluvium
Anagen effluvium is the rapid loss of hair during the active growth phase, most commonly caused by chemotherapy, radiation therapy, or exposure to toxic chemicals. Unlike telogen effluvium, where hairs are shed gradually over months, anagen effluvium causes hair to fall out rapidly, often within days or weeks of exposure to the triggering agent.
The mechanism is direct damage to the rapidly dividing cells in the hair matrix. Because 85 to 90 percent of scalp hairs are in the anagen phase at any given time, the loss can be dramatic and nearly complete. The encouraging news is that anagen effluvium is almost always fully reversible. Once the causative exposure ends, the follicles recover and regrow hair, though the new hair may differ in texture or color from the original.
Transplant candidacy: Hair transplantation is not indicated for anagen effluvium, as the condition resolves on its own after the causative agent is removed.
Choosing the Right Treatment for Your Type of Alopecia
The critical takeaway from this overview is that accurate diagnosis must precede treatment. The treatments that work brilliantly for androgenetic alopecia, including finasteride, minoxidil, and hair transplant surgery, may be ineffective or inappropriate for autoimmune, scarring, or reactive forms of hair loss. Conversely, the immunomodulatory treatments essential for alopecia areata would provide no benefit for androgenetic alopecia.
A thorough evaluation by a specialist who understands the full spectrum of hair loss conditions is the most important investment you can make. The right diagnosis leads to the right treatment, and the right treatment leads to real results.
At Bellevue Hair Doctor, our evaluation process includes a detailed clinical history, scalp examination, trichoscopic analysis, and, when indicated, blood work or scalp biopsy to arrive at an accurate diagnosis. From there, we build a treatment plan tailored to your specific condition, whether that involves medical therapy, PRP treatments, surgical restoration, or a combination approach.
Related Articles

Understanding Male Pattern Baldness: Causes, Stages & Solutions
A clinical guide to androgenetic alopecia in men, covering the Norwood scale, genetic factors, and all available treatment options.

Female Hair Loss: Common Causes and Treatment Options
Why women experience hair thinning and loss, from hormonal shifts to medical conditions, and which treatments deliver real results.

FUE vs FUT: Which Hair Transplant Method Is Right for You?
A detailed comparison of Follicular Unit Extraction and Follicular Unit Transplantation covering scarring, recovery, cost, and graft yield.
Schedule Your Free Consultation
Have questions about hair loss or treatment options? Our board-certified specialists are here to help.